-
Posted By arooba rehman
-
-
Comments 0
Vasectomy is a widely used method of permanent male contraception, but it is often misunderstood—especially when it comes to how it affects sperm production. A common assumption is that vasectomy stops the body from producing sperm altogether. In reality, the process is far more nuanced. Exploring Vasectomy and Sperm Production Mechanisms helps clarify how the male reproductive system adapts after the procedure and why hormonal and physiological functions largely remain intact.
Understanding Normal Sperm Production
To fully grasp the impact of vasectomy, it is important to first understand how sperm is produced. Sperm production, or spermatogenesis, occurs in the seminiferous tubules of the testicles. This process is continuous and regulated by hormones, primarily testosterone and follicle-stimulating hormone (FSH).
Once produced, sperm travels through a series of structures:
- Epididymis (where sperm matures and is stored)
- Vas deferens (which transports sperm during ejaculation)
- Urethra (through which semen is expelled)
This entire system works seamlessly to ensure fertility under normal conditions.
What Happens During a Vasectomy?
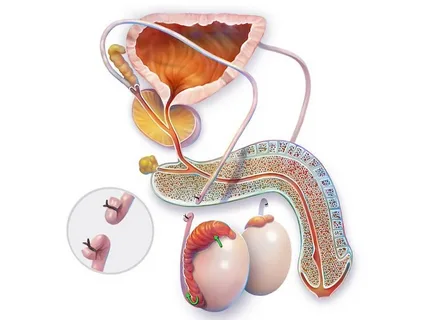
A vasectomy involves cutting, sealing, or blocking the vas deferens. This prevents sperm from traveling from the epididymis to the urethra. Importantly, the testicles themselves are not altered, and the hormonal system remains unchanged.
From the perspective of Vasectomy and Sperm Production Mechanisms, the key takeaway is that sperm production continues even after the pathway for sperm transport is interrupted.
Does Vasectomy Stop Sperm Production?
No, vasectomy does not stop sperm production. The testicles continue to produce sperm at roughly the same rate as before the procedure. However, because the vas deferens is blocked, sperm cannot exit the body during ejaculation.
Instead, the body naturally reabsorbs the unused sperm. This is a normal physiological process that occurs even in men who have not undergone vasectomy, as not all produced sperm is ejaculated.
The Role of the Epididymis After Vasectomy
After a vasectomy, sperm accumulates in the epididymis, the structure responsible for sperm maturation and storage. Over time, the body adjusts by:
- Breaking down excess sperm
- Reabsorbing cellular components
- Maintaining a balance between production and clearance
This adaptive mechanism ensures that there is no harmful buildup of sperm within the reproductive system.
Hormonal Regulation Remains Unchanged
One of the most important aspects of Vasectomy and Sperm Production Mechanisms is that hormonal function is unaffected. Testosterone, the primary male sex hormone, continues to be produced by the testicles and released into the bloodstream.
As a result:
- Libido remains stable
- Secondary sexual characteristics are preserved
- Energy levels and mood are not impacted by the procedure
This distinction is crucial, as it separates vasectomy from procedures that directly affect hormone production.
What Happens to Sperm at the Cellular Level?
After vasectomy, sperm cells undergo a natural lifecycle within the body. Since they cannot be ejaculated, they are broken down by immune cells and reabsorbed. The components of sperm—such as proteins and lipids—are recycled by the body.
In some cases, the immune system may recognize sperm as foreign and produce antibodies against them. While this is a normal response, it typically has no noticeable health effects and does not impact overall well-being.
Pressure and Adaptation in the Testicles
In the initial period following vasectomy, there may be a slight increase in pressure within the epididymis due to continued sperm production. However, the body quickly adapts through:
- Reduced sperm production rates (in some individuals)
- Increased reabsorption efficiency
- Structural adjustments within the epididymis
These changes help maintain equilibrium and prevent long-term complications.
Long-Term Changes in Sperm Production
Over time, subtle changes may occur in the rate of sperm production. Some studies suggest a slight decrease in spermatogenesis due to feedback mechanisms, but this does not have any clinical significance since fertility is already intentionally eliminated.
From a Vasectomy and Sperm Production Mechanisms perspective, the key point is that the reproductive system remains biologically active, even though its function in reproduction is effectively disabled.
Impact on Semen Composition
Another common misconception is that vasectomy significantly alters semen volume. In reality, sperm makes up only about 2–5% of total semen volume. The majority comes from the seminal vesicles and prostate gland.
After vasectomy:
- Semen volume remains largely unchanged
- Appearance and consistency are similar
- Ejaculation feels the same
The only difference is the absence of sperm, which is not noticeable without microscopic analysis.
Reversibility and Sperm Function
Although vasectomy is intended to be permanent, reversal procedures (vasovasostomy) can sometimes restore the connection between the vas deferens. However, success rates vary and depend on factors such as:
- Time since vasectomy
- Surgical technique used
- Presence of anti-sperm antibodies
Even when reversal is successful, sperm production may not fully return to pre-vasectomy fertility levels, highlighting the importance of considering vasectomy as a long-term decision.
Myths and Misconceptions
There are several myths surrounding Vasectomy and Sperm Production Mechanisms:
- Myth: Vasectomy stops sperm production
Reality: Sperm production continues normally - Myth: Vasectomy affects masculinity
Reality: Hormones and sexual function remain unchanged - Myth: Sperm buildup is harmful
Reality: The body safely reabsorbs sperm without adverse effects
Addressing these misconceptions is essential for helping patients make informed choices.
Clinical Significance
Understanding sperm production after vasectomy is not just a matter of curiosity—it has practical implications for patient care. For example:
- Explaining continued sperm production helps manage expectations
- Clarifying reabsorption reduces anxiety about “blocked” sperm
- Educating patients improves compliance with follow-up testing
In Vasectomy and Sperm Production Mechanisms, knowledge empowers both patients and healthcare providers to approach the procedure with confidence.
Conclusion
The relationship between vasectomy and sperm production is a clear example of how the human body adapts to surgical intervention. While the procedure effectively prevents sperm from being included in semen, it does not disrupt the underlying biological processes of sperm production or hormonal regulation.
By understanding Vasectomy and Sperm Production Mechanisms, patients can appreciate that vasectomy is not about shutting down the reproductive system, but rather redirecting its function in a safe and controlled way. This distinction reinforces the procedure’s safety, effectiveness, and suitability as a long-term contraceptive option.
FAQs
1. Does sperm production stop after a vasectomy?
No, sperm production continues normally in the testicles. The sperm is simply reabsorbed by the body instead of being ejaculated.
2. Where does sperm go after a vasectomy?
Sperm is broken down and reabsorbed by the body, primarily in the epididymis, without causing harm.
3. Does vasectomy affect testosterone levels?
No, vasectomy does not impact testosterone production. Hormone levels, libido, and sexual function remain unchanged.

